OCD and eating disorders are two distinct but complex mental health conditions that severely impact quality of life. Although both are separate conditions, they often coexist.
According to the National Eating Disorder Association, Around 15% to 18% of people with eating disorders also struggle with OCD. The comorbidity is stronger in subtypes of eating disorders, such as anorexia nervosa, where obsessive characteristics and obsessive rituals are common.
However, this overlapping often leads to extreme distress in everyday life activities and causes confusion in diagnosis. It ultimately makes the treatment more challenging.
Understanding the connection between these disorders is important for effective treatments.
The Connection between OCD and Eating Disorders
In both OCD and eating disorders, the main point is performing “ritual behaviors” which provide quick, temporary relief. However, it eventually strengthens the cycle by teaching the brain that the only way to feel safe is to perform the behavior.
In obsessive-compulsive disorder, people experience irrational thoughts, known as obsessions and compulsions, to elevate anxiety. These thoughts can occur in several ways, such as fear of germs, symmetry, and doubts. Individuals experiencing this condition feel compelled to ease their obsessions by constantly washing hands, arranging and re-arranging things, and seeking reassurances. Obsessions and compulsions are time-consuming and often disturb the normal functioning of life.
Want to get rid off this compulsion? try our OCD treatment services Today.
Eating behavior severely affects physical and emotional health and the relationship with food, which can be life-threatening. A person may experience an intrusive thought about body image or weight. To neutralize that anxiety, they engage in a “compulsion” such as restrictive eating, over-exercising, or calorie counting.
However, every individual’s experience with this disorder is different and varies depending on its type. This can lead to dangerous eating behaviors. These behaviors can seriously affect the ability to get the nutrition your body needs. It can also harm the heart, digestive system, bones, teeth, and mouth.
However, in both conditions, the “compulsions” provide temporary relief, but it ultimately strengthens the cycle by teaching the brain that the only way to feel safe is to perform the ritual behaviors.
The Biological and Genetic Link
OCD and eating disorders are not just related by their behaviors; they also share some biological roots.
- OCD and eating disorders are strongly linked together due to imbalances in neurotransmitters such as serotonin, which regulates mood, anxiety, and impulse control.
- This is also linked in brain connectivity as the orbitofrontal cortex and the caudate nucleus signal the brain and are involved in habit formation. It is a very common habit in both disorders.
Read More About : Understand the Biology of OCD
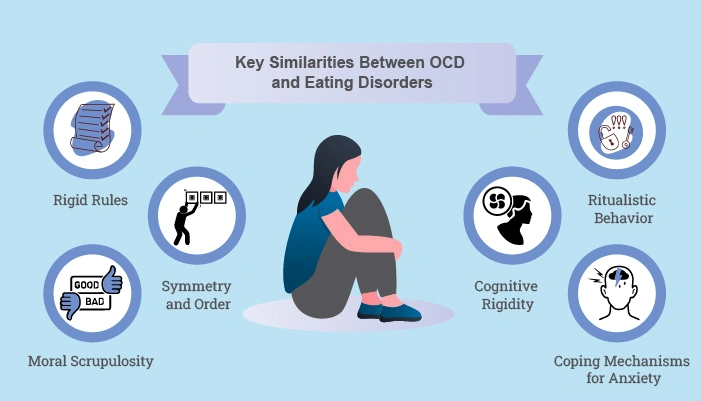
Key Similarities Between OCD and Eating Disorders
OCD and Eating Disorders are separate mental health conditions, but they both have behaviors that can look remarkably similar, including:
These parallel traits underline the complex link between the two conditions.
- Rigid Rules: OCD and eating disorders both involve “rules” that cannot be changed. For an individual with OCD, it might be washing hands three times, and for someone with an eating disorder, it might be never eating after 6:00 PM.
- Symmetry and Order: Many people with eating disorders struggle with symmetry, which is also very common in OCD. It can be manifested as arranging food perfectly on a plate or cutting it into exact, equal pieces.
- Moral Scrupulosity: People experiencing both OCD and eating disorders often have a sense of “goodness” or “badness” attached to actions. People in this state feel like eating food can be a moral failure. Also, OCD individuals might also feel like they have committed a “sin”.
- Ritualistic Behavior: People experiencing these conditions engage in ritualistic behaviors that need to be performed to relieve anxiety. In OCD, it can be repetitive cleaning or checking, while in eating disorders, it can be restrictive eating or excessive exercise.
- Cognitive Rigidity: It is one of the major symptoms of both OCD and eating disorders. Individuals in this state have difficulty adapting to new situations or changing their behaviors. This rigidity can lead to unhealthy eating patterns or make one perform compulsive rituals.
- Coping Mechanisms for Anxiety: People experiencing these conditions often use coping tools to reduce anxiety, trauma, or stress. The need to control food intake or maintain routines can only become a way to manage overwhelming feelings. However, these mechanisms ultimately worsen the symptoms.
Key Differences Between OCD and Eating Disorders
Despite similarities, both conditions remain different; here are some of the differences that help in diagnosing the condition.
- Content of intrusive thoughts: Obsessions with OCD revolve around contamination, damage, order, or moral concerns and are not primarily focused on weight or shape. Whereas in eating-disorders, the thoughts revolve around weight, food, calories, and body image, with intense fear of gaining weight or becoming “out of control” around food. However, both conditions have food-related fear, but with differences.
- Ego-dystonic vs ego-syntonic: the main difference is that eating disorders are often ego-syntonic, meaning people may see their behaviors as part of their identity and may not recognize them. In contrast, OCD is typically ego-dystonic, which means people with OCD often recognize their compulsive behaviors as unreasonable but are unable to stop them.
What are the Risk Factors of OCD & Eating Disorders?
There are several factors that may contribute to the development of both OCD and eating disorders, including genetics, family history, and mental health conditions, such as anxiety and depression.

1. Societal Pressures
Societal pressure to get to an idealized body type often drives individuals to develop disordered eating habits. These are harmful for people in different communities, such as people who may face discrimination based on their body size, race, or gender. The stigma of being fat can increase the obsessive need to control one’s weight. It eventually leads to compulsive behaviors like excessive exercise, dieting, or purging.
2. Racism and Sexism
People also face significant challenges while dealing with eating disorders and OCD. Women are more likely to experience these pressures, while people with different tone colors, such as dark skin, may also face the complexities of cultural discrimination.
3. Trauma and Abuse
A person with a history of abuse, neglect, or trauma is also vulnerable to developing OCD and eating disorders. Also, people having traumatic experiences also need to control food intake or engage themselves in compulsive behaviors in a way to cope with their overwhelming emotions.
Diagnostic Challenges
Diagnosing the co-occurrence of OCD and eating disorders comes with several challenges.
Both conditions have similarities, which make the diagnoses difficult to differentiate between them. These intervening conditions can overshadow one another, which leads to misdiagnosis and causes difficulties with effective treatments. For example, an individual might receive treatment for an eating disorder while their undiagnosed OCD symptoms remain unaddressed, or vice versa.
However, to diagnose these conditions, mental health professionals typically gather detailed histories and follow specific guidelines to accurately identify these conditions.
Treatment Approaches
OCD and eating disorders are highly curable, with the right combination of medication and therapies.
Medications, such as selective serotonin reuptake inhibitors (SSRIs), antidepressants, or anti-anxiety medications, may be recommended for co-occurring conditions. These medications are commonly used alongside therapy for better outcomes, with treatment plans tailored to individual needs.
Also, there are some therapy options:
Cognitive-Behavioral Therapy (CBT): It is an effective treatment for both eating disorders and obsessive-compulsive disorder. CBT helps people identify and challenge negative thought patterns, develop healthier coping strategies, and reduce obsessive behaviors. Through CBT, people learn to reframe their thoughts and develop a more balanced view of food, body image, and anxiety.
Exposure and Response Prevention (ERP): It is particularly effective for Obsessive Compulsive Disorder (OCD). ERP involves gradually exposing individuals to feared situations or thoughts without engaging in obsessional behaviors. This process helps treat OCD and helps individuals build patience to reduce their reliance on ritual behavior as a coping mechanism.
Support Groups and Family Involvement: It plays an important role in the recovery process. The group therapy sessions provide a supportive environment for individuals to share their experiences and learn from others facing similar challenges. Family therapy helps loved ones understand the impact of OCD and eating disorders and provides support throughout the recovery journey.
For eating disorders, Dialectical Behavior Therapy (DBT) may be used to manage emotional regulation and coping strategies.
Additionally, some lifestyle changes help in reducing stress, such as meditation, deep breathing exercises, journaling, and maintaining routines. These changes help individuals manage anxiety and reduce the impact of obsessive thoughts and compulsive behavior.
When to Seek Help
If you feel like your symptoms are getting out of control and cannot be controlled on their own, reaching out to a mental health professional is the first step. Here is when you need to speak with a professional:
- Obsessions and compulsions interfere with daily life activities
- Thoughts about food, body image, or rituals consume excessive time
- If you experience sudden weight changes or feel like you are dieting excessively
- Physical health begins to decline
- Feelings of shame, guilt, or isolation become overwhelming
Note: Early intervention is crucial, as eating disorders can lead to serious health risks.
Take the First Step Toward Recovery at Renewed Mental Health Group
Understanding the connection between obsessive-compulsive disorder (OCD) and eating disorders is difficult for both individuals affected by these conditions. If you or someone you know is struggling with OCD or an eating disorder, it’s important to recognize that these conditions can often coexist and worsen each other’s impact on mental and physical health.
At Renewed Mental Health Group, we have a team of certified mental health professionals who provide compassionate treatments with multidisciplinary approaches. Our top-rated experts offer a safe and nurturing environment where you can talk about your issues without the fear of judgment.
Your mental health matters!
Book your consultations now!